A Retrospective Analysis of Pain Changes and Opioid Use Patterns Temporally Associated with a Course of Chiropractic Care at a Publicly Funded Inner-city Facility
A Retrospective Analysis of Pain Changes and Opioid Use Patterns Temporally Associated with a Course of Chiropractic Care at a Publicly Funded Inner-city Facility
SOURCE: J Can Chiropr Assoc 2022 (Aug); 66 (2): 107–117
| OPEN ACCESS |
Steven Passmore, Hons BKin, MS, DC, PhD, Quinn Malone, BSc, MSc1, Christian Manansala, BSc, DC, MSc, Spencer Ferbers, BSc,
E. Audrey Toth, DC, Gerald M. Olin, BSc, DC, CDir
Faculty of Kinesiology and Recreation Management,
University of Manitoba,
102- Frank Kennedy Centre,
420 University Crescent,
Winnipeg, MB, R3T 2N2 Canada

FROM: Kazis et. al, BMJ Open 2019
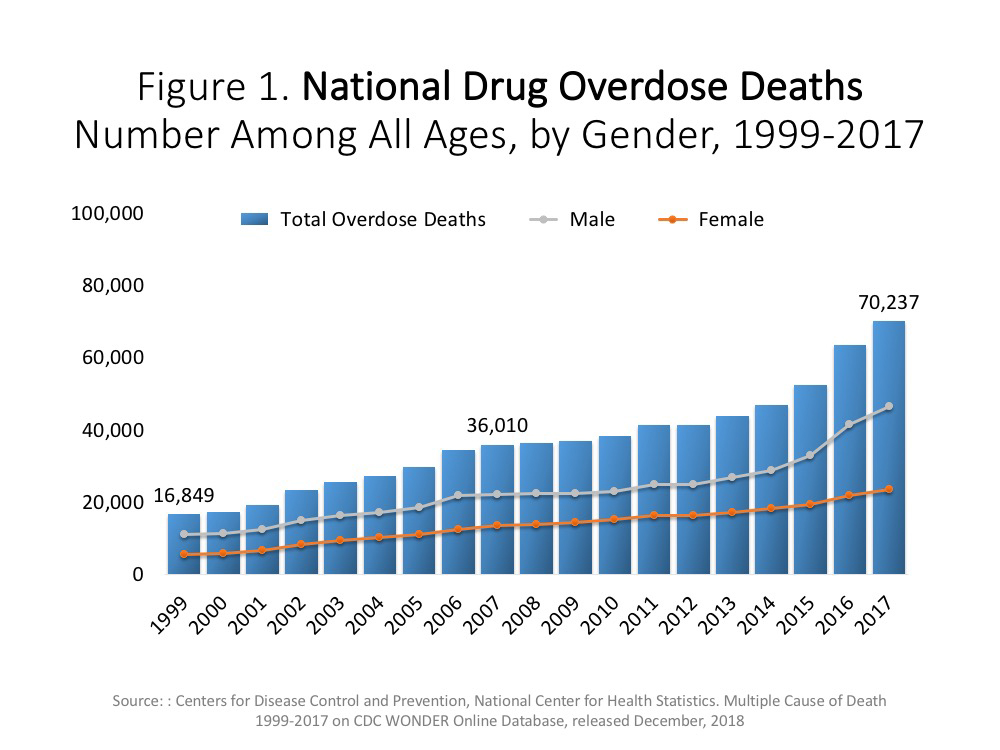
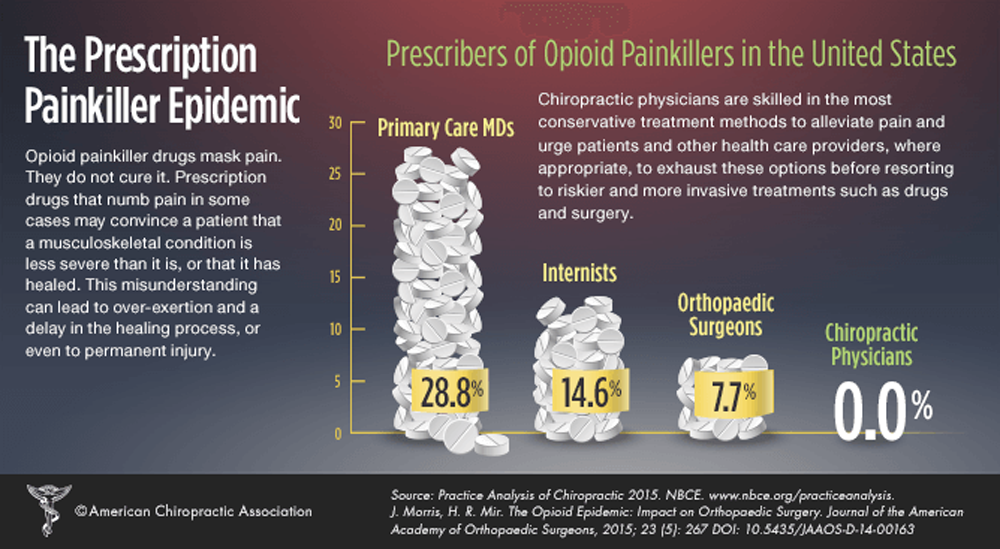
Background: Non-pharmacologic treatment, including chiropractic care, is now recommended instead of opioid prescriptions as the initial management of chronic spine pain by clinical practice guidelines. Chiropractic care, commonly including spinal manipulation, has been temporally associated with reduced opioid prescription in veterans with spine pain.
Purpose: To determine if chiropractic management including spinal manipulation was associated with decreased pain or opioid usage in financially disadvantaged individuals utilizing opioid medications and diagnosed with musculoskeletal conditions.
Methods: A retrospective analysis of quality assurance data from a publicly funded healthcare facility was conducted. Measures included numeric pain scores of spine and extremity regions across three time points, opioid utilization, demographics, and care modalities.
Results: Pain and opioid use significantly decreased concomitant with a course of chiropractic care.
There is more like this @ our:
OPIOID EPIDEMIC Section and the: