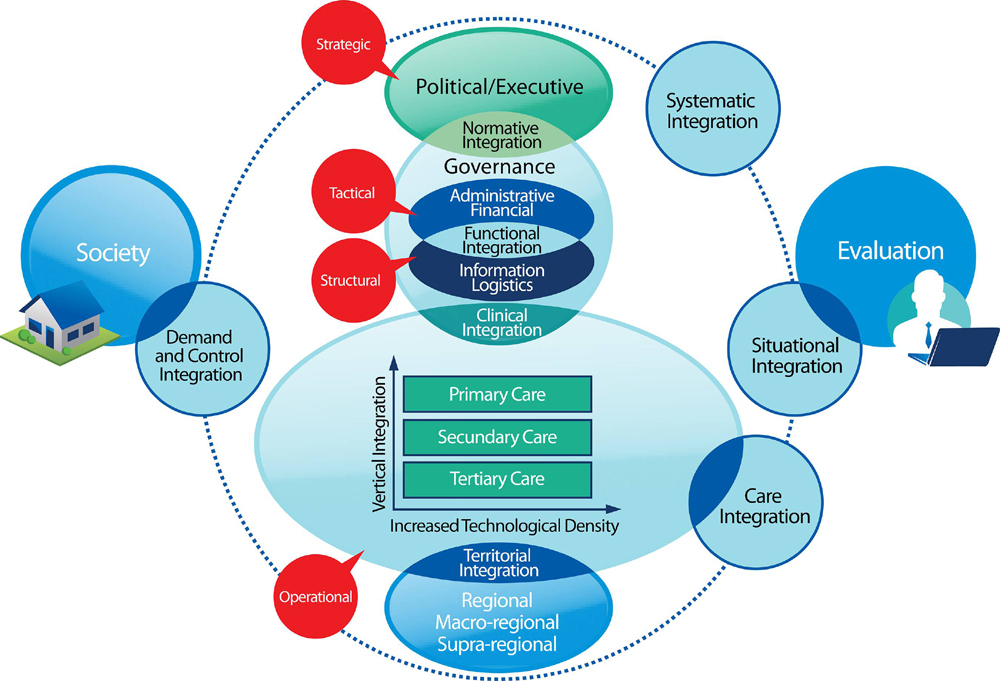
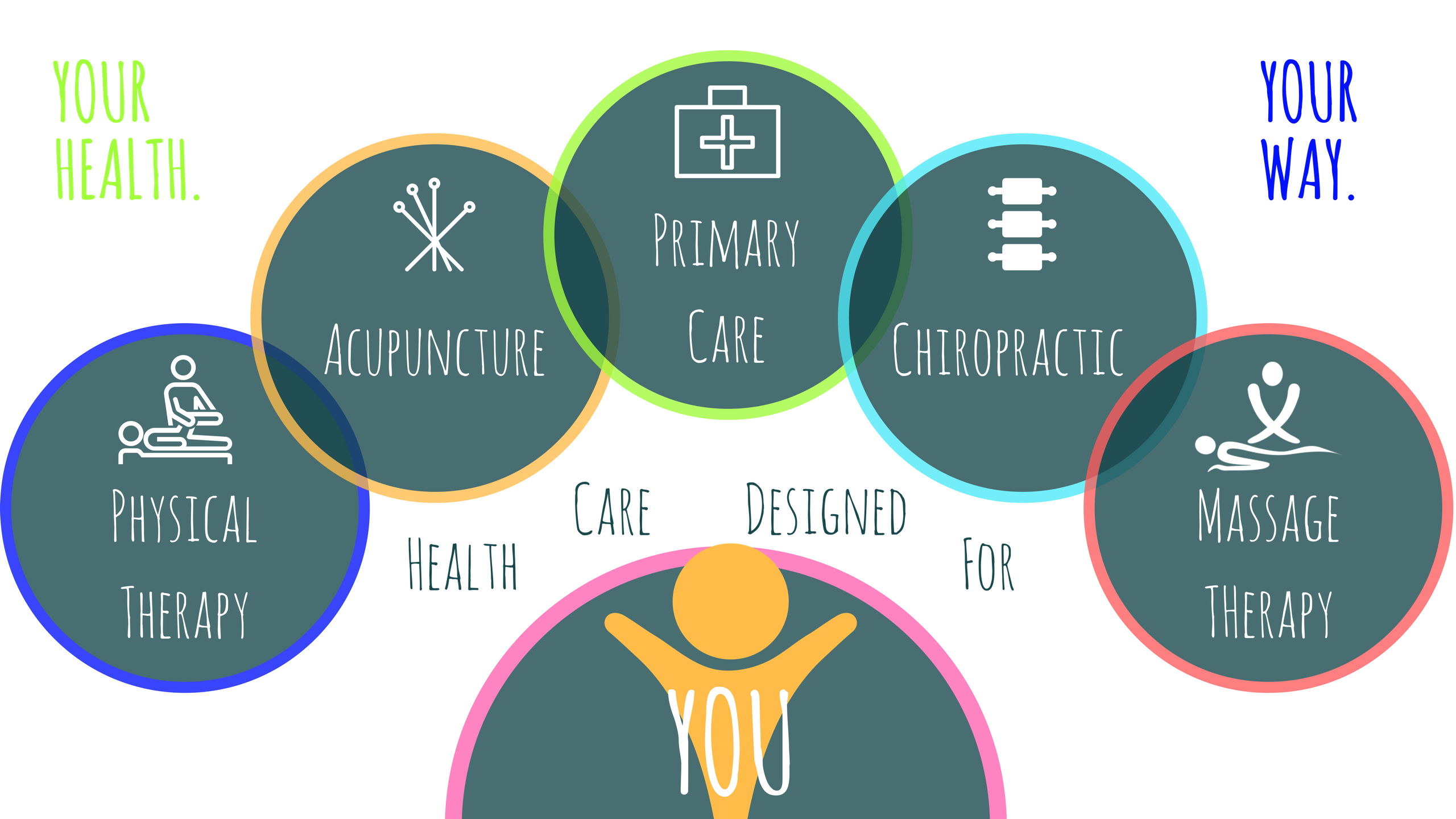
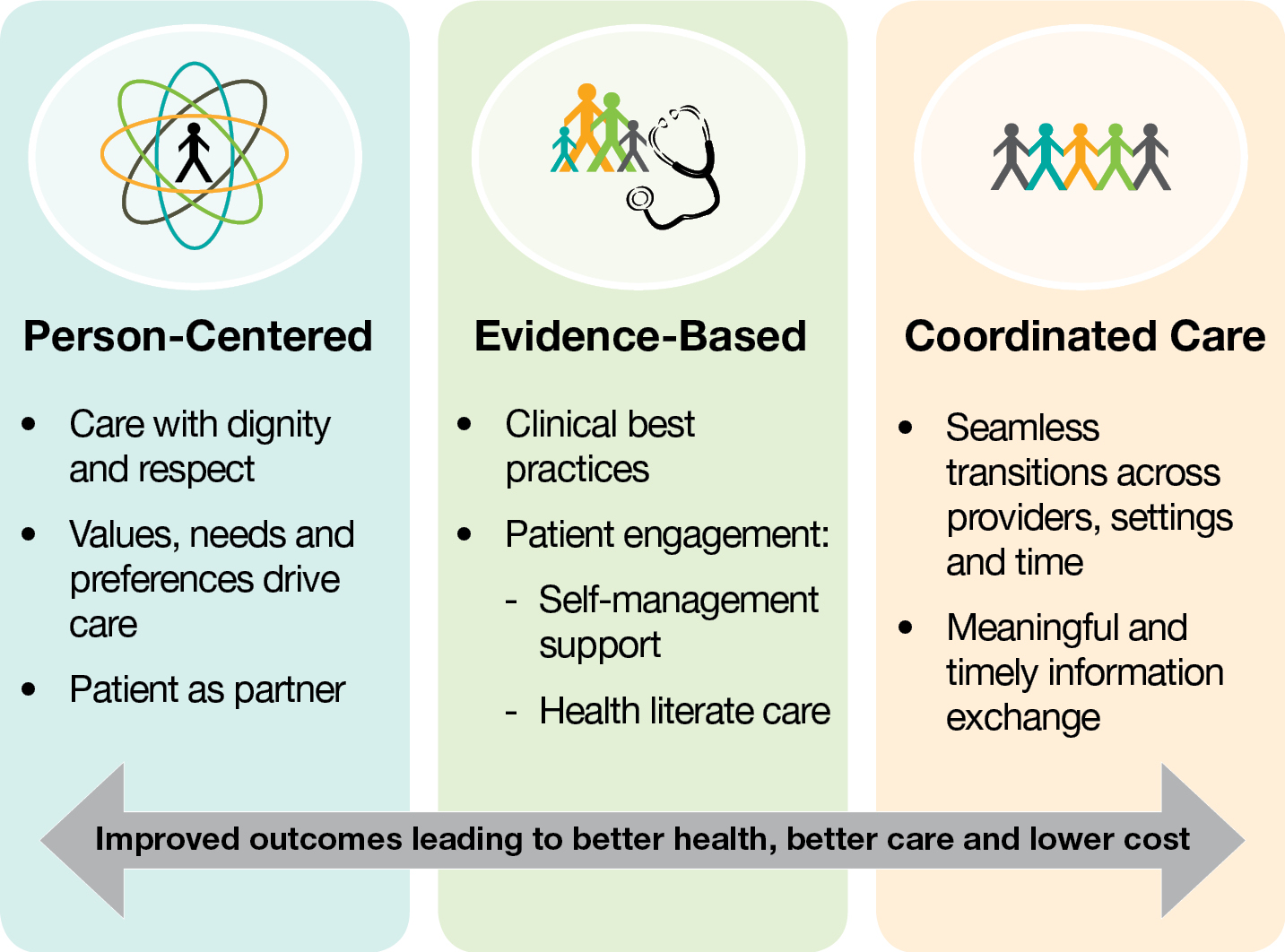
Developing Integrative Primary Healthcare Delivery
Developing Integrative Primary Healthcare Delivery: Adding a Chiropractor to the Team
SOURCE: Explore (NY). 2008 (Jan); 4 (1): 18–24
Michael J. Garner, MSc, Michael Birmingham, PhD, Peter Aker, MSc, DC, David Moher, PhD,
Jeff Balon, DC, MD, Dirk Keenan, DC, and Pran Manga, PhD
Carlington Community and Health Services,
Ottawa, Ontario, Canada.

BACKGROUND: The use of complementary and alternative medicine has been increasing in Canada despite the lack of coverage under the universal public health insurance system. Physicians and other healthcare practitioners are now being placed in multidisciplinary teams, yet little research on integration exists.
OBJECTIVE: We sought to investigate the effect of integrating chiropractic on the attitudes of providers on two healthcare teams.
DESIGN: A mixed methods design with both quantitative and qualitative components was used to assess the healthcare teams. Assessment occurred prior to integration, at midstudy, and at the end of the study (18 months).
SETTING: Multidisciplinary healthcare teams at two community health centers in Ottawa, Ontario, participated in the study.
PATIENTS/PARTICIPANTS: All physicians, nurse practitioners, and degree-trained nurses employed at two study sites were approached to take part in the study.
INTERVENTION: A chiropractor was introduced into each of the two healthcare teams.
MAIN OUTCOME MEASURES: A quantitative questionnaire assessed providers’ opinions, experiences with collaboration, and perceptions of chiropractic care. Focus groups were used to encourage providers to communicate their experiences and perceptions of the integration and of chiropractic.
RESULTS: Twelve providers were followed for the full 18 months of integration. The providers expressed increased willingness to trust the chiropractors in shared care (F value = 7.18; P = .004). Questions regarding the legitimacy (F value = 12.33; P < .001) and effectiveness (F value = 11.17; P < .001) of chiropractic became increasingly positive by study end.
There are more articles like this @ our: