Treatment Targets of Exercise for Persistent Non-specific Low Back Pain: A Consensus Study
Treatment Targets of Exercise for Persistent Non-specific Low Back Pain: A Consensus Study
SOURCE: Physiotherapy 2021 (Sep); 112: 78–86
Lianne Wood, Annette Bishop, Martyn Lewis, Rob J E M Smeets, Gert Bronfort, Jill A Hayden, Nadine E Foster
Primary Care Centre Versus Arthritis,
School of Primary, Community and Social Care,
Faculty of Medicine and Health Sciences,
Keele University,
Newcastle-under-Lyme ST5 5BG, UK
FROM: Br J Sports Med 2020
Objectives: Despite several hundred previous randomised controlled trials (RCTs), the key treatment targets of exercise for persistent non-specific low back pain (NSLBP) remain unclear. This study aimed to generate consensus about the key treatment targets of exercise interventions for patients with NSLBP.
Design: Consensus was generated using modified nominal group technique in two, sequential, workshops. The results of a previous systematic review informed the first, national, workshop idea generation and the results of this workshop informed the second, international, workshop. The authors generated a starting list of 30 treatment targets from the systematic review. A pre-specified consensus threshold of 75% was used in the voting stage.
Participants: Workshop participants included people with experience of using exercise to manage their persistent NSLBP, clinicians who prescribe exercise for persistent NSLBP, and researchers who design and evaluate exercise interventions in RCTs. All participants generated, voted and ranked the treatment targets in each workshop using an online platform.
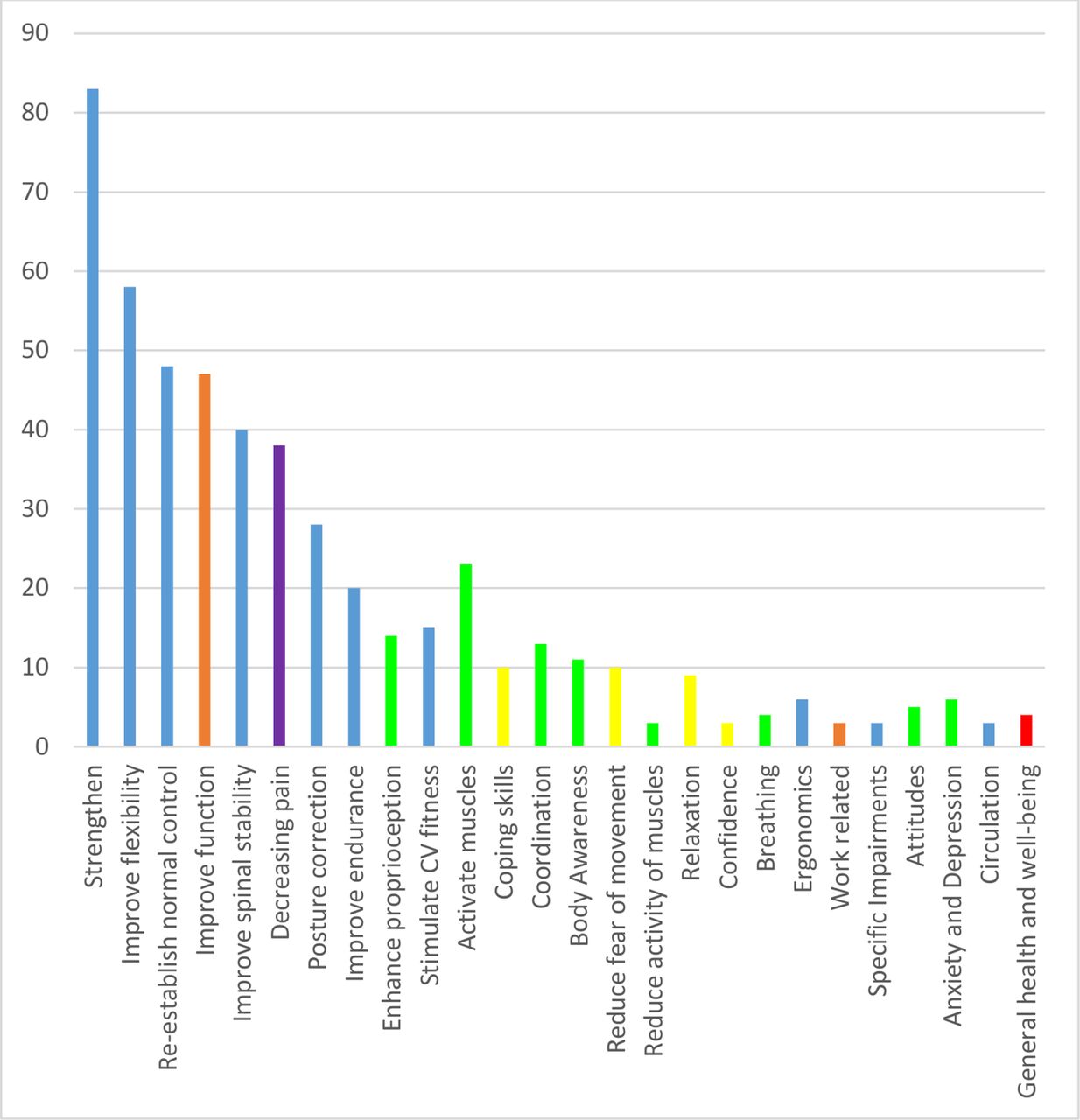
Results: A total of 39 participants contributed to the consensus (15 in the national workshop and 24 in the international workshop), comprising two people with NSLBP, six clinicians and 31 researchers/clinicians. A total of 40 exercise treatment targets were generated, and 25 were retained after voting and ranking. The prioritised targets of exercise for persistent NSLBP were: improving function, improving quality of life, reducing pain, meeting patient-specific goals and reducing fear of movement.
There is more like this @ our:
LOW BACK PAIN Section and the: