Chiropractic Care for Workers with Low Back Pain
SOURCE: Workers Compensation Research Institute (May 17, 2022)
Dongchun Wang, Kathryn Mueller, Randall Lea, M.D., Donald R. Murphy
Related Topics: Medical Costs, Outcomes for Injured Workers, Physical Medicine, Utilization
Cambridge, MA, May 17, 2022 — Today, the Workers Compensation Research Institute (WCRI) announced the release of a new study on chiropractic care for low back pain. The study reveals substantial variation in the use of chiropractic care across 28 states and offers insights into the patterns and outcomes of chiropractic care.
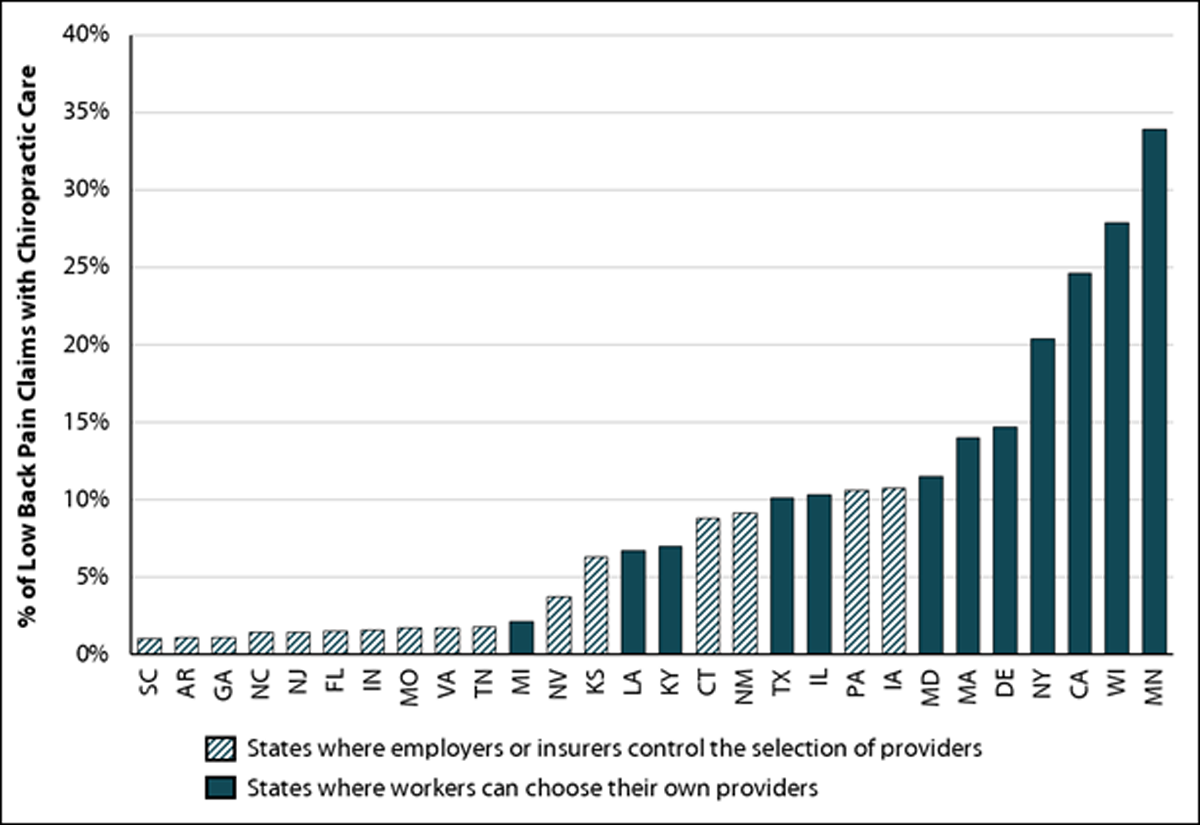
“Chiropractors often participate in the delivery of physical medicine services for low back pain, but few workers received chiropractic care in states where employers or insurers control the selection of providers,” said John Ruser, WCRI’s president and CEO. “This study will be helpful for policymakers and stakeholders who are interested in re-evaluating the role of chiropractors, especially those who have been adopting evidence-based practices and contributing to cost-effective care.”
This study, Chiropractic Care for Workers with Low Back Pain, describes the prevalence of chiropractic care and provider patterns of physical medicine treatment for workers with low back pain. It provides some evidence as to how different provider patterns of physical medicine treatment are associated with variations in overall medical and indemnity costs, and the duration of temporary disability. The study also looks at the utilization of medical services, including magnetic imaging studies, opioid prescriptions, and pain management injections.
The following is a sample of the study’s key findings:
There are more articles like this @
The prevalence of chiropractic care varied substantially across the 28 study states. States that give employers control of selecting medical providers were among the states with the lowest prevalence of chiropractic care.
When chiropractors are involved in care, they alone may provide physical medicine care or deliver physical medicine care in conjunction with other non-chiropractic physical medicine providers. Based on the experience of 16 states with prevalent chiropractic care, 12 percent of workers with low back pain received physical medicine care exclusively from chiropractors, and 17 percent received physical medicine treatment from chiropractors and other non-chiropractic providers, concurrently or sequentially.
Claims with care provided exclusively by chiropractors were associated with lower costs and shorter duration of temporary disability than a set of claims with similar characteristics where care was exclusively provided by non-chiropractic providers.
 |
The data used for this study are from the WCRI Detailed Benchmark/Evaluation database, which includes more than 2 million open and closed claims from 28 states, with injuries from October 1, 2015, through September 30, 2017, and detailed medical transactions up through March 31, 2019. The 28 states are Arkansas, California, Connecticut, Delaware, Florida, Georgia, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maryland, Massachusetts, Michigan, Minnesota, Missouri, Nevada, New Jersey, New Mexico, New York, North Carolina, Pennsylvania, South Carolina, Tennessee, Texas, Virginia, and Wisconsin.
To learn more about this study or to download a copy, visit WCRI’s website at https://www.wcrinet.org/reports/chiropractic-care-for-workers-with-low-back-pain. Dongchun Wang, Kathryn L. Mueller, Donald R. Murphy, and Randall D. Lea authored the study.
About WCRI:
The Workers Compensation Research Institute (WCRI) is an independent, not-for-profit research organization based in Cambridge, MA. Organized in late 1983, the Institute does not take positions on the issues it researches; rather, it provides information obtained through studies and data collection efforts, which conform to recognized scientific methods. Objectivity is further ensured through rigorous, unbiased peer review procedures. WCRI’s diverse membership includes employers; insurers; governmental entities; managed care companies; health care providers; insurance regulators; state labor organizations; and state administrative agencies in the U.S., Canada, Australia, and New Zealand.

Leave A Comment