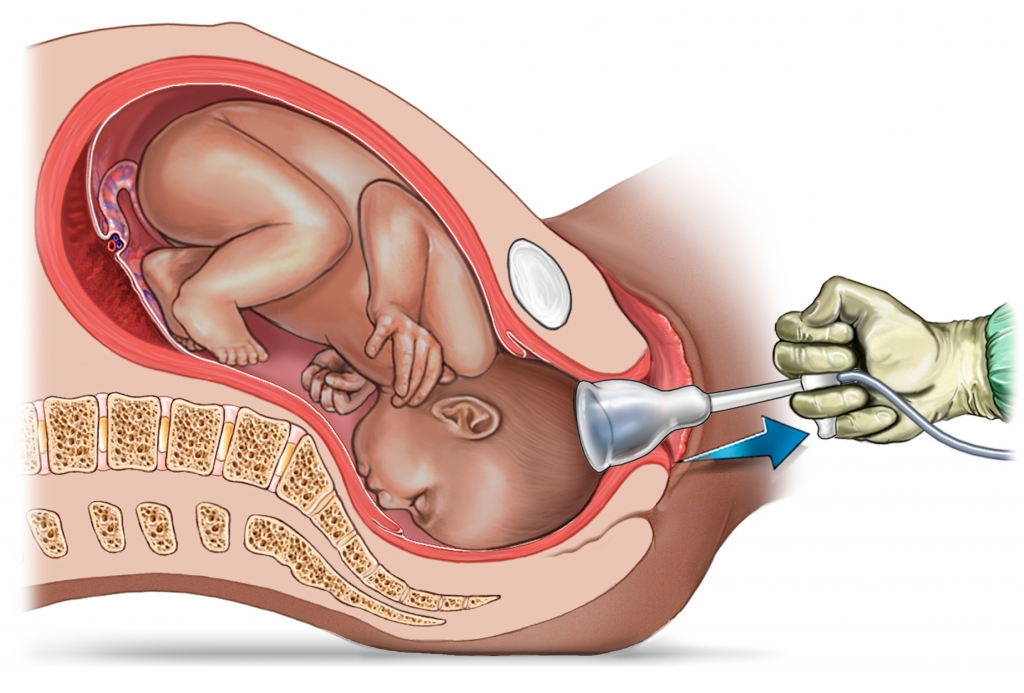
Manual Therapy for the Pediatric Population
Manual Therapy for the Pediatric Population: A Systematic Review
SOURCE: BMC Complement Altern Med. 2019 (Mar 13); 19 (1): 60
Carol Parnell Prevost, Brian Gleberzon, Beth Carleo, Kristian Anderson, Morgan Cark and Katherine A. Pohlman
Palmer College of Chiropractic,
4777 City Center Parkway,
Port Orange, FL, 32129, USA.
BACKGROUND: This systematic review evaluates the use of manual therapy for clinical conditions in the pediatric population, assesses the methodological quality of the studies found, and synthesizes findings based on health condition. We also assessed the reporting of adverse events within the included studies and compared our conclusions to those of the UK Update report.
METHODS: Six databases were searched using the following inclusion criteria: children under the age of 18 years old; treatment using manual therapy; any type of healthcare profession; published between 2001 and March 31, 2018; and English. Case reports were excluded from our study. Reference tracking was performed on six published relevant systematic reviews to find any missed article. Each study that met the inclusion criteria was screened by two authors to:
(i) determine its suitability for inclusion,
(ii) extract data, and
(iii) aasess quality of study.
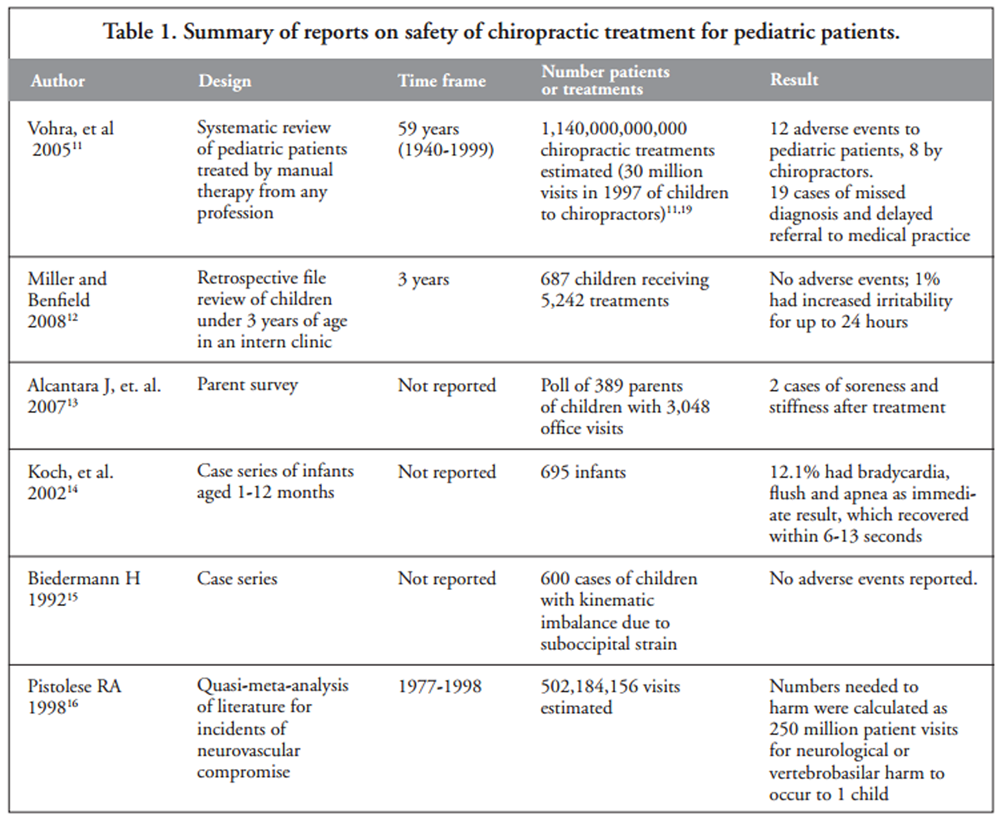
RESULTS: Of the 3,563 articles identified, 165 full articles were screened, and 50 studies met the inclusion criteria. Twenty-six articles were included in prior reviews with 24 new studies identified. Eighteen studies were judged to be of high quality. Conditions evaluated were: attention deficit hyperactivity disorder (ADHD), autism, asthma, cerebral palsy, clubfoot, constipation, cranial asymmetry, cuboid syndrome, headache, infantile colic, low back pain, obstructive apnea, otitis media, pediatric dysfunctional voiding, pediatric nocturnal enuresis, postural asymmetry, preterm infants, pulled elbow, suboptimal infant breastfeeding, scoliosis, suboptimal infant breastfeeding, temporomandibular dysfunction, torticollis, and upper cervical dysfunction. Musculoskeletal conditions, including low back pain and headache, were evaluated in seven studies. Twenty studies reported adverse events, which were transient and mild to moderate in severity.
There are more articles like this @ our: