Epidural Steroid Injections: Are long-term Risks Worth Short Term Benefits?
SOURCE: ACA News ~ February 2014
By William Morgan, DC
Outpatient procedures are where the money is in medicine these days. Such procedures are invasive treatments that are not quite surgery but are not conservative care either. Non-surgical procedura lists are falling over themselves at an alarming rate to learn these lucrative businesses. This is true in several medical specialties: cardiac catheterization labs, GI endoscopies and colonoscopies, interventional radiology procedures, PMR pain procedures, urologic cystoscopies, chiropractic manipulation under anesthesia, epidural steroid injection therapies and many other pain procedures. If utilized correctly, these procedures may be valuable tools in the treatment of patients by preventing more invasive procedures, and in the case of cystoscopies and colonoscopies, aid in the early detection of cancer.
These procedures can be done quickly with assembly line efficiency and are very profitable for the physicians. In the case of epidural steroid injections (ESI), a ten-minute epidural procedure will generally yield anywhere from a couple hundred to a couple thousand dollars, though I have heard of a series of three epidurals going for as much as $8,000. Furthermore, if done in an outpatient facility, the physician does not have to split the fees with a hospital, and the insurance company does not need to pay the higher costs that normally accompany hospital-based procedures. Last year in the United States, the Centers for Medicare and Medicaid Services (CMS) paid for nearly nine million ESI. This number may not appear surprising at first, but when you consider that ESI therapies are neither approved by the FDA [1] nor recommended by the manufacturers [2] due to reports of severe adverse events, it becomes alarmingly relevant. Note that the CMS number is not the total number of ESI performed in the United States. The nine million number represents only those ESI paid for by CMS. When we add in the number of ESI performed in the DOD, VA, workers’ compensation systems and private insurance, that number could conceivably be in the tens of millions.
While it is true that ESI are not FDA approved, Medicare, Medicaid, workers’ compensation and most other insurers continue to pay hundreds of millions of dollars per year for this controversial procedure.
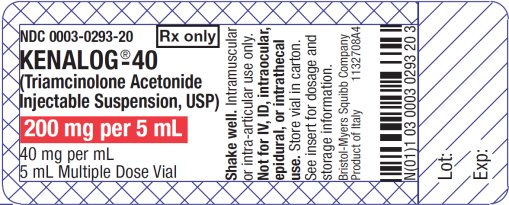
Ironically, on every vial of Kenalog (a popular steroid used for epidural injections) there is actually a warning against its use for epidural injections, yet proceduralists continue to use it.
There are more articles like this @ our:
Although there is inadequate evidence to support the high use of ESI in the United States, it remains a very popular growth industry. This is partially due to ESI being purported to reduce the number of spine surgeries. However, studies like one performed by Arden, et al. [3] show that ESI did not offer sustained benefits nor did it reduce the need for spinal surgery. Arden’s study did show that there was a transient reduction of symptoms in patients with sciatica. Carette, et al. performed a separate study with similar results. [4]
In the ten-year period between 2000 and 2010, the use of ESI increased 160 percent. Dr. Manchikanti, chairman of the American Society of Interventional Pain Physicians, stated:
He attributed this remarkable increase in spinal injections to the increased number of patients seeking pain relief and the financial incentives afforded to the treating physicians.
SOURCE: Read the rest of this Full Text article now!

Leave A Comment