Can Neurotransmitter Status Affect the Results of Exercise-Based Scoliosis Treatment? Results of a Controlled Comparative Chart Review
SOURCE: Alternative & Integrative Medicine 2014 (Nov 20); 3: 177
Mark W Morningstar, Aatif Siddiqui,
Brian Dovorany and Clayton J Stitzel
Natural Wellness & Pain Relief Center
8293 Office Park Dr.,
Grand Blanc, MI 48439, USA
Idiopathic scoliosis has long been held as a purely orthopedic spinal deformity without a known origin. Hence all treatment of scoliosis has involved physical methods exclusively to treat the condition, whether by bracing, surgery, or exercise-based methods. Over the last several years many authors have introduced etiological concepts of scoliosis involving multiple biochemical central nervous system pathways, such as neurotransmitter imbalances. The purpose of this study is to evaluate how these neurotransmitter imbalances affect patients’ ability to participate in a scoliosis therapy program and the ability of the resultant radiographic changes to be maintained. Two groups of patients performed baseline neurotransmitter testing, and completed a short-term chiropractic rehabilitation program for scoliosis. One group additionally participated in a nutrient program designed to rebalance their neurotransmitter levels, while the second group declined. Both groups were evaluated 6 months after the completion of their rehabilitation program to evaluate Cobb angle changes
Keywords Chiropractic; Nutrition; Scoliosis; Spine; Rehabilitation
From the Full-Text Article:
Introduction:
Scoliosis is historically thought of as a purely biomechanical or orthopedic disorder of the spine wherein the spine curves greater than 10 degrees on radiographic assessment. [1] Conventional treatments of scoliosis have been entirely based upon this model of scoliosis, whether it be bracing or surgery. Both of these treatments entirely focus upon the spine curvature, and attempt to straighten or stabilize the spine throughout the human growing years.
There are more articles like this @ our:
Although these treatments are still the gold standard of treatment in the United States, there have been several researchers who have written extensively about the neurological and hormonal precursors to scoliosis. Machida was among the first to describe the onset of scoliosis following artificially created melatonin deficiencies in animal experiments. [2–4] Other authors have suggested that melatonin signaling dysfunctions may be a more logical explanation for the development of scoliosis as compared to frank melatonin deficiencies. [5] In addition to melatonin, leptin resistance has also been described as integral in scoliosis development. [6]
Burwell et al. [7] have described a “Double Neuro-Osseous Theory” of scoliosis development, which identifies asymmetrical signaling within the sympathetic nervous system, resulting to asymmetrical proximal long bone and rib growth. This, they believe, forces the body to compensate for asymmetrical growth by inducing spinal counter-rotations and translations.
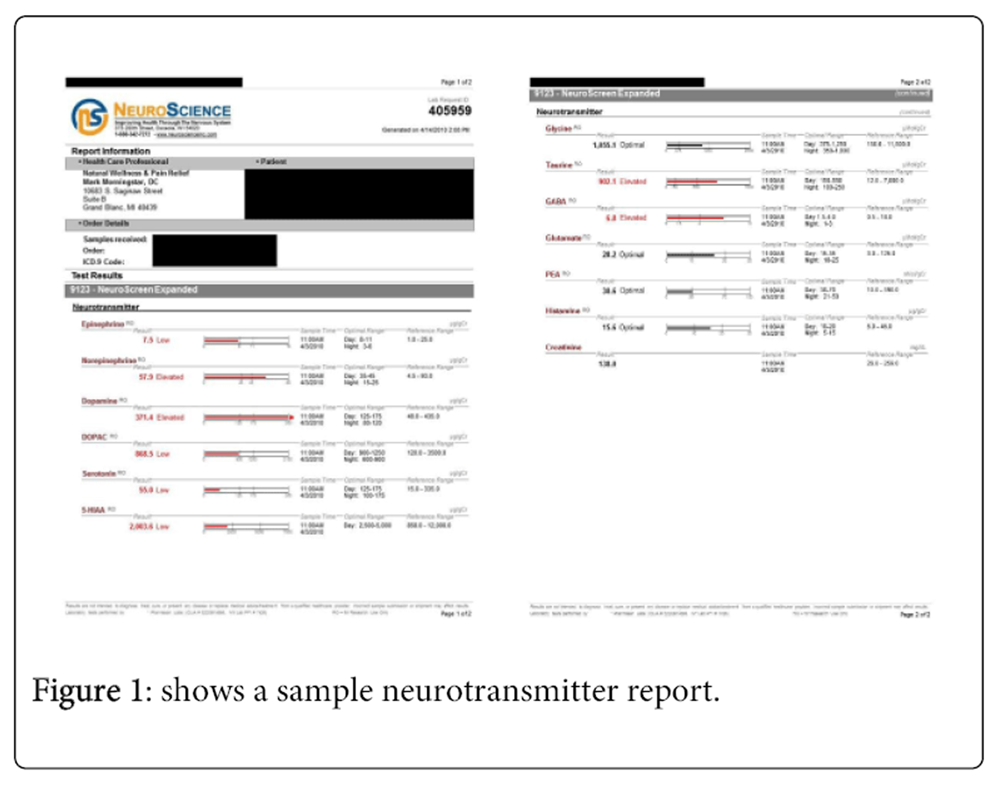
Regardless of the fact that the exact mechanisms behind scoliosis development are still unclear, what is clear is that there is a host of identified biochemical abnormalities in patients with idiopathic scoliosis, observations for which conventional treatments in the U.S. do not account. Recently, Morningstar suggested that patients with idiopathic scoliosis demonstrate trends of abnormal neurotransmitter imbalances not shown in non-scoliotic patients. [8] This purpose of this study is to determine if correcting these identified neurotransmitter imbalances in patients with idiopathic scoliosis result in better outcomes from exercise-based scoliosis treatment.
Read the rest of this Full Text article now!


Leave A Comment